Findings of a second Homecare Association member survey, August 2021
Summary
Following our report in July 2021 on shortage of homecare workers, we conducted a second survey of Homecare Association members in August 2021. The aim was to test whether the findings in July were due to short-term issues related to COVID-19 self-isolation policies at the time, or to more persistent problems.
Responses were received from 843 homecare providers, large and small, state-funded and private-pay funded, across all regions of England. This was a record number of responses to a member survey, indicating the high level of concern among employers about inadequate workforce capacity to meet demand.
Key findings were as follows:
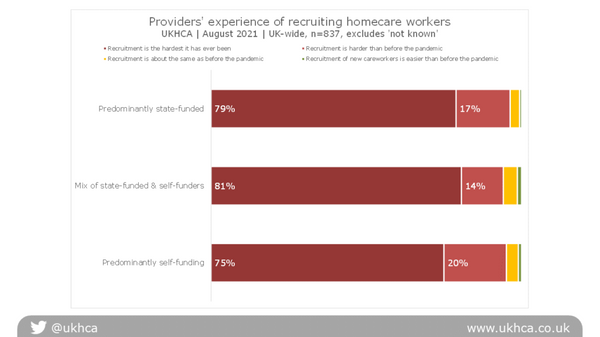
- 95% of homecare providers said that recruitment was harder than before the COVID-19 pandemic, with the majority (78%) saying that recruitment was “the hardest it has ever been”. There were not substantial regional differences.
- Providers serving predominantly the private-pay part of the market reported similar challenges to those serving predominantly the state-funded part of the market.
- 65% of homecare providers said that more careworkers were leaving their jobs than before the pandemic, including 29% who said that more careworkers were leaving than ever before. Just 4% said that fewer careworkers were leaving than before the pandemic.
- 89% of providers stated that demand for their services had increased or significantly increased over the previous two months. Just 2% said that demand had reduced or significantly reduced.
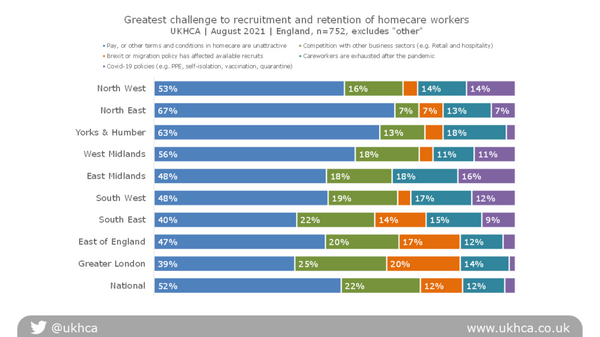
- Careworkers’ pay and available terms and conditions of employment were said to be the greatest challenge to recruiting and retaining homecare workers, with 46% of employers describing that as the most significant issue. This is, of course, closely linked to how the homecare sector is funded by the State, and what private individuals arranging their own care are willing and able to pay. Consistent patterns were seen across regions, with some variation.
- 38% of providers said they were unable to take on new work, with 57% saying they could take on some but not all new work.
- 29% of providers said they were handing some work back, with 1% saying they were handing all work back. 70% were continuing to meet existing need.
ITV News reported on these findings and filmed careworkers and care managers talking emotionally about the challenges they are facing, saying they are the worst they have ever experienced.
Lord Bethell dismissed our research as “anecdote”, when asked by Baroness Brinton in the House of Lords about government plans to help older and disabled people adversely affected by shortages of homecare workers.
Whilst the government is apparently denying that workforce capacity in homecare is inadequate to meet demand, some NHS hospitals are reporting critical incidents due to shortage of beds and inability to discharge people to community and social care services.
Though hospital discharge data are no longer reported in public, we know from our members’ experience across the country that demand for homecare is currently exceeding supply. When people cannot be moved back to the community from hospital in a timely manner, it reduces available beds for new admissions and lengthens waits for vital treatment.
A new survey from the Directors of Adult Social Services (ADASS) states that 13% of people are being offered care and support, such as residential care that they would not have chosen, due to recruitment and retention issues.
Vaccination as a condition of deployment is on the horizon for homecare, as the government has issued a new consultation on whether or not to extend vaccination requirements to other health and care settings for COVID-19 and also for influenza.
As strong supporters of vaccination, we remain keen to ensure that as many homecare workers as possible receive both doses of the COVID-19 vaccine, as there is good evidence this protects the recipient from serious illness.
We believe, however, that persuasion is likely to be more effective than compulsion at improving uptake, whilst minimising loss of workforce capacity.
Furthermore, recent evidence suggests that the delta variant of COVID-19 may be spread by vaccinated as well as un-vaccinated people, so the argument that vaccination reduces risk to others may not stand up. Other infection prevention and control measures, such as PPE, regular testing, ventilation, and thorough cleaning schedules, are also crucial and continue to be implemented across the homecare sector.
We have repeatedly raised concerns about the risk of older and disabled people being left without care at home, if vaccination rates among the homecare workforce do not increase above current average levels of 81.8% for the first dose and 69.8% for the second dose, and careworkers lose their jobs as a result. The averages mask substantial variation, with some London boroughs recording vaccination rates of homecare workers as low as 57% for the first dose and 38% for the second dose.
We could therefore lose 20 per cent or more homecare workers at a time when supply of careworkers is already inadequate to meet rising demand.
Workforce losses could be far worse if influenza vaccination also becomes a condition of deployment. Last year, ‘flu vaccine uptake among social care workers in care homes was around 33%. Figures have not been reported for homecare. Influenza vaccine supply issues last year meant that some homecare workers were turned away multiple times and eventually gave up.
The government’s recent announcement about funding reform for social care makes no provision to address the deep-seated workforce issues affecting homecare and the wider sector. This is very disappointing.
The Homecare Association continues to call on the government to:
- Fund social care adequately so that homecare workers are paid fairly for the skilled roles they perform, and at least on a par with equivalent public sector roles.
- End the practice of councils and the NHS of purchasing homecare “by-the-minute”, alternatively focusing on achieving the outcomes people want.
- Support development of an expert-led workforce strategy for social care and a 10-year workforce plan, aligned with the NHS People Plan.
- Create a professional register for careworkers in England, covering all paid social care workers in both regulated and unregulated care services. Registration of careworkers needs to be adequately funded and carefully implemented.

About the collection method and response rate
Responses were collected though a self-selecting on-line survey of UKHCA member organisations between 5 August 2021 and 10 August 2021.
UKHCA runs a number of on-line surveys with our member organisations, and this received the highest completion rate of any survey undertaken, which suggests to us how critical this issue is for employers.
843 respondents completed the survey. A further 34 started the survey, but did not answer all the questions and were excluded. The completion rate was therefore 96.1%.
In our analysis of answers to individual questions we have excluded the very small number of responses who said that they did not know (or preferred not to state) the answer to one or more individual questions. This accounted for between 0.1% and 7% of responses to individual question. This accounts for different sample sizes reported in some questions.
Organisations completing the survey
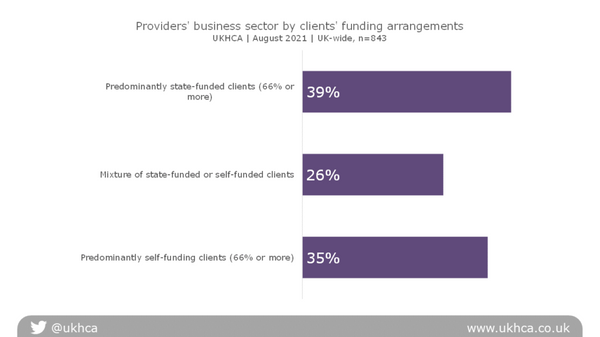
The survey was completed by providers serving either predominantly state-funding or self-funding clients, and a mixture of both. Our analysis of the difference between these sectors suggests that while those in the privately-funded market reported slightly less extreme responses to the questions, they are facing similar problems.
Results
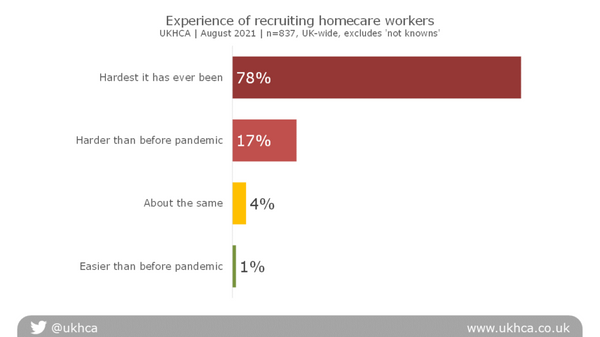
Recruitment of careworkers
95% of homecare providers said that recruitment was harder than before the pandemic, with the majority of respondents (78%) saying that recruitment was “the hardest it has ever been”.
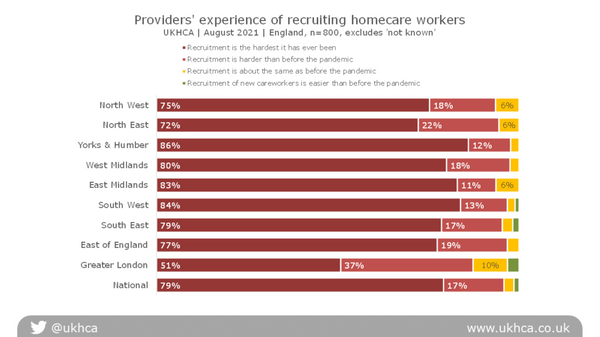
An analysis by government regions in England shows that, with the exception of Greater London, where the weighting of extremes was not quite so severe, this is a national issue.
Neither is the difficulty recruiting careworkers confined solely to the state-funded sector, where recruitment of homecare workers is generally regarded as harder than in the private-pay part of the market.
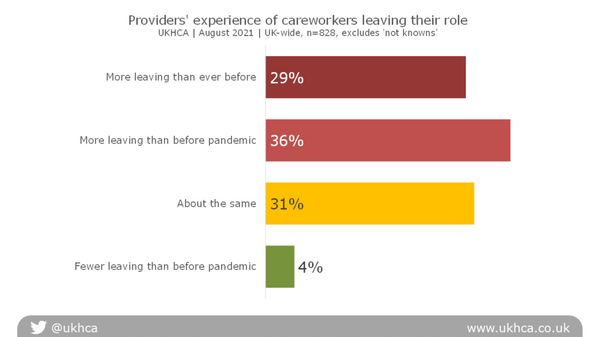
Careworkers leaving their role
65% of homecare providers said that more careworkers were leaving their jobs than before the pandemic, including 29% who said that more careworkers were leaving than ever before. Just 4% said that fewer careworkers were leaving than before the pandemic.
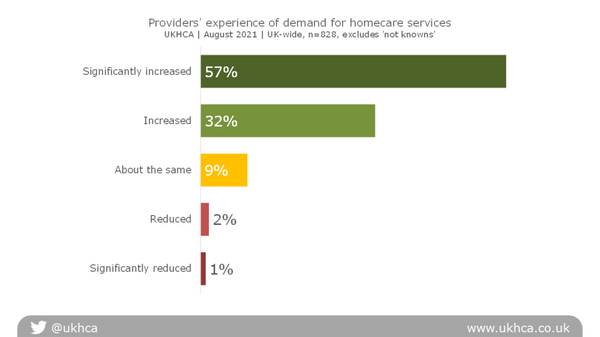
Demand for homecare services
89% of providers stated that demand for their services had increased or significantly increased over the previous two months. Just 2% said that demand had reduced or significantly reduced.
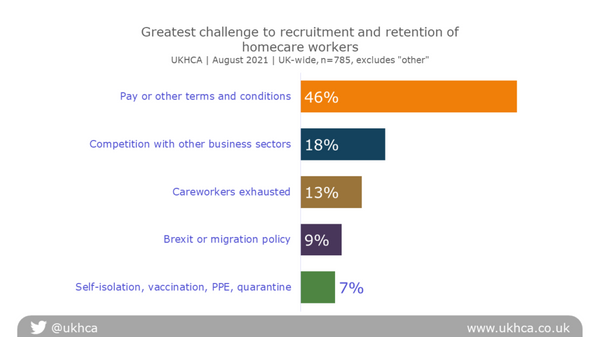
Reasons for challenges in recruitment and retention
Providers reported that the key challenges to recruitment and retention were:
- Pay, terms and conditions of employment which do not fairly reward skill and experience
- Competition with other business sectors
- Exhaustion and burn-out of careworkers
- Brexit or migration policy
- COVID-19 related policies, such as self-isolation, PPE, vaccination, quarantine
Careworkers’ pay and available terms and conditions of employment were the greatest challenge to recruiting and retaining homecare workers, with 46% of employers describing that as the most significant issue.
This is, of course, closely linked to how the homecare sector is funded by the State, and what private individuals arranging their own care are willing and able to pay.
The option ‘other’ represented a range of views, including employers stating that the pressures were so interlinked that it was difficult to distinguish between them.
The regional breakdown of these data shows a reasonably consistent pattern, with some variation.
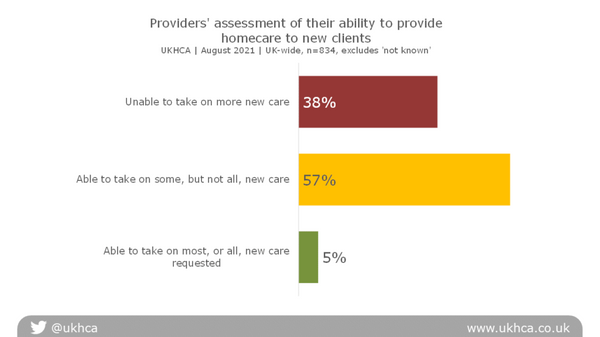
Providers’ assessment of their ability to provide homecare to new clients
95% of providers reported that they were unable to take on some or all new clients, of which 38% said they could not currently take on any new clients.
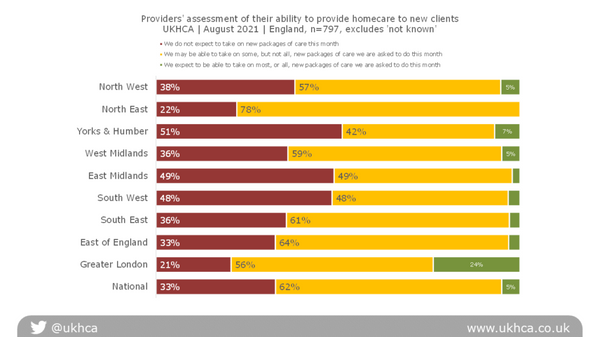
Similar patterns were observed across most regions, with the South West and East Midlands reporting the lowest ability to provide homecare to new clients.
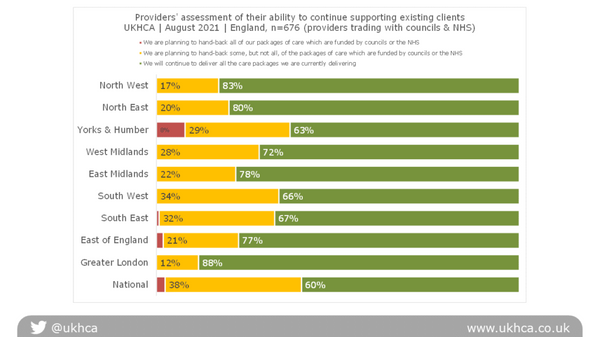
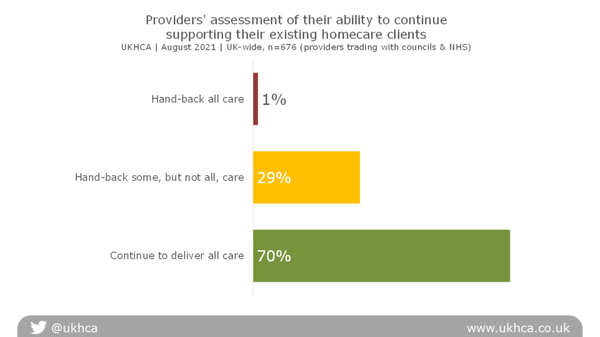
Providers’ assessment of their ability to continue supporting their existing homecare clients
Please note that this question was only asked of homecare providers who delivered services to local councils or the NHS, accounting for a lower sample size.
30% of providers reported that they are handing some or all of their existing work back to councils or the NHS, as they have inadequate staff to continue to deliver care safely.
Issues with workforce capacity are visible in every region. A higher proportion of providers in Yorkshire and Humberside and the East of England reported handing all work back than in other areas.