People at the Heart of Care - our views on the White Paper
We all want to live well at home, surrounded by those important to us, and connected to our communities.

It is very encouraging that home-based support and care is at the heart of the vision for social care articulated in the Adult Social Care Reform White Paper. This is what we wanted to see.
Building on the principles of the Care Act 2014, the paper talks about listening to people receiving support; personalisation; prevention; choice and control; information to help navigate the health and care system; support for informal carers; support for the professional workforce; innovation and technology; and oversight of the system.
All of these are great aspirations that resonate with those receiving and giving support and care.
We are grateful for the widespread consultation and opportunity to contribute. It is our genuine hope that this vision will become a reality over the next 10 years.
These aspirations will, however, remain just aspirations unless the vision, plan for implementation, and investment are aligned.
And this is where our concerns lie.
Whilst the proposals contain welcome additional funding for a range of areas, including housing (£300m); innovation (£30m); technology (£150m); informal carers (£25m); workforce (£500m); and testing new ways of providing information (£5m), which will be valued by many, they do not address underlying systemic issues.
Government continues to pour billions into the black hole of NHS acute hospitals. There’s no sign of a meaningful shift in investment towards supporting people in the community, addressing inequalities or tackling the social determinants of health.
Homecare receives only 4% of the amount invested in the NHS.
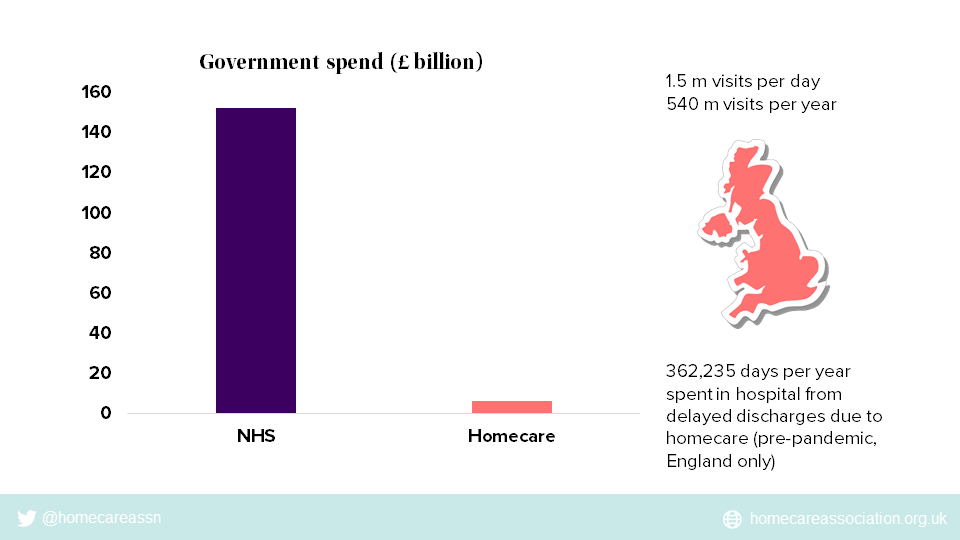
Currently, we neglect people in the community, wait until they reach crisis point, then blue light them to an ambulance queue. When they eventually get into hospital, they struggle to get out again, due to inadequate capacity in community and social care.
This does not seem an intelligent way to use limited resources.

The White Paper recognises the need to shift the demand curve and focus on prevention and we strongly support this intention. We are, however, a long way from this, particularly in the state-funded part of the market, and it’s hard to see how this will change in the current funding environment.
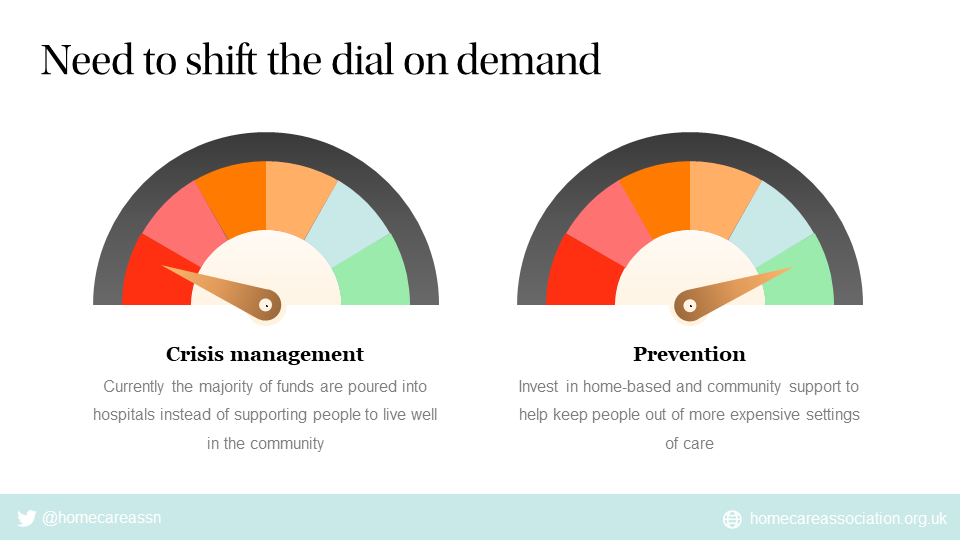
Demand for home-based support and care is outstripping supply. Unmet need is high and rising. Recruitment and retention of careworkers in homecare is the hardest it has ever been.
Shortage of careworkers risks harm to older and disabled people. It is also very stressful for careworkers, who may feel they are unable to meet needs adequately as they are so stretched, when their motivation is to improve lives.
Funding cuts to councils over many years have led to rationing and poor approaches to commissioning and purchasing of homecare. In turn, this has resulted in poor pay, terms and conditions for the workforce.
The government’s answer to this is to say they are putting the Care Quality Commission in charge of oversight of local authorities.
The Homecare Association has long believed that quality in homecare is heavily dependent on the way homecare is commissioned and purchased. We have argued that regulatory focus on provision of care alone is not enough to ensure that people receive high quality care and achieve the outcomes they desire. So we are pleased that CQC has been given these new responsibilities.
It appears, however, that CQC will have no enforcement powers in their role in local authority oversight. All they can do is identify and describe problems, give ratings and write advisory reports.
If a local authority is so cash-strapped that it is driven to purchasing homecare by the minute at fee rates which are too low to enable quality, compliance or sustainability of provision, how will a CQC advisory report change anything?
The ability of providers to charge a fair price for care to self-funders to help maintain solvency is undermined by the policy to encourage further use of section 18 (3) of the Care Act 2014.
Simple calculations based on announcements already made suggest that remaining funds available for the fair cost of care are likely to be at least 10 times too low.
The Competition and Markets Authority identified that £1 billion extra funding would be needed across the UK for councils to pay fee rates which cover the costs care homes incur.
In our Homecare Deficit Report 2021, we calculated that £1.7 billion extra funding would be needed across the UK for public organisations to purchase homecare at fee rates that allow careworkers to be paid £11.14 per hour. This is equivalent to a NHS Band 3 healthcare assistant or a supermarket worker.
Effectively forcing providers to accept local authority fee rates, which will likely remain inadequate due to inadequate central government funding, substantially increases risk. How does the government expect market stability if investment does not support the policy intention?
The care market is already hanging in the balance.
Providers are projecting 8-10% increases in costs this coming year, driven largely by wage inflation in the wider economy, beyond the 6.6% increase in the national living wage. Other costs such as National Insurance contributions, insurance and fuel for driving are also rising and it remains unknown if providers will have to bear the additional costs of COVID-19 related PPE after March 2022.
Central government has made it clear that councils must cover increases in unit costs and demographic pressures by efficiency savings and increasing council tax. It will not be possible for councils to come close to covering inflationary pressures of 8-10%.
We call on the government to walk the talk on levelling up and provide sustainable funding for community and social care, especially in areas of greatest deprivation.
Our Homecare Deficit report provided clear evidence that local authority areas with the highest indices of deprivation have the lowest fee rates.
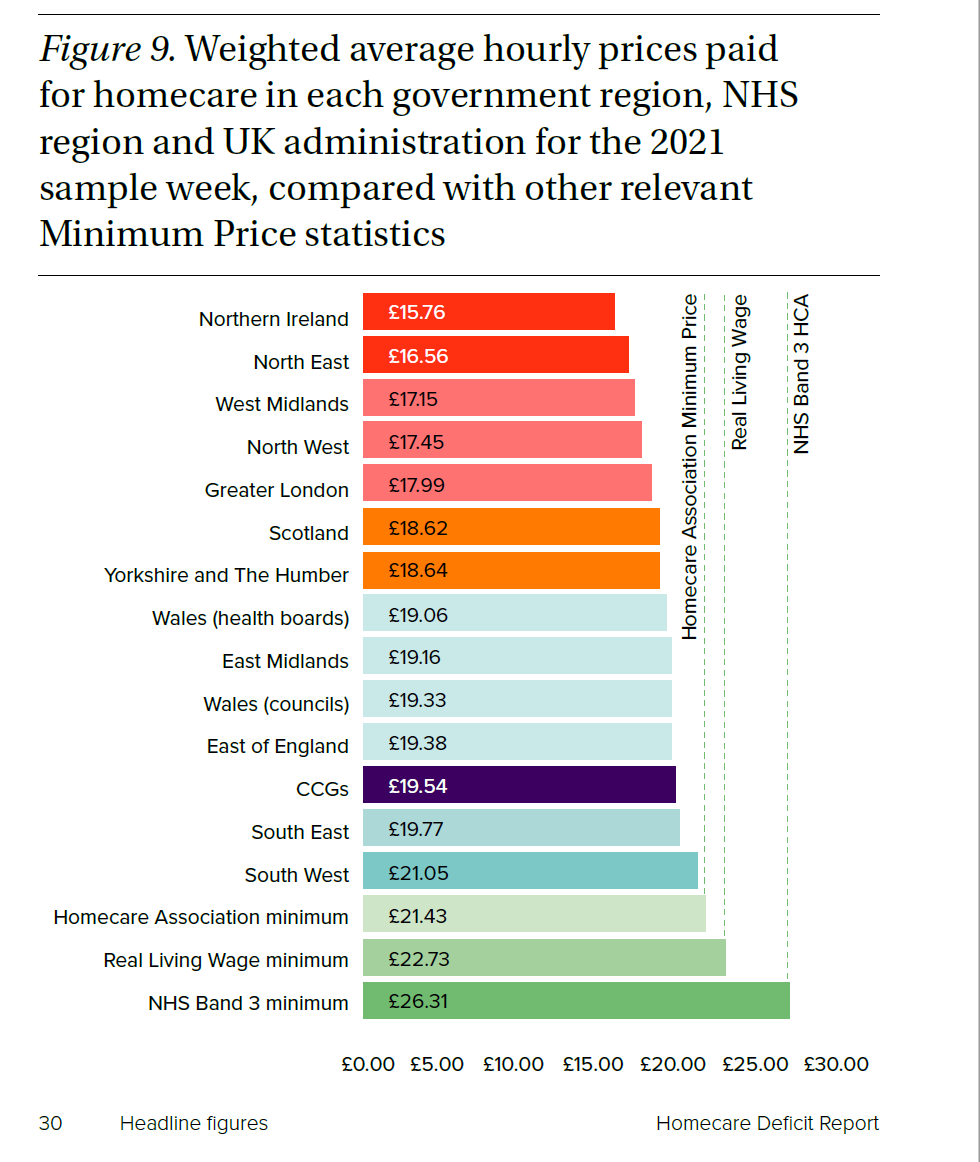
We need to see adequate investment in our workforce so they receive appropriate training and supervision as well as fair pay, terms and conditions of employment.
The £500m allocated for workforce equates to £111 per person per year. All additional funding is positive but this is not game-changing and the proposals are unlikely to have a significant impact on recruitment and retention.
And finally we need to see better cross-government working to link social care with education, housing, employment, environment, business and the economy, so we can focus more on improving the social determinants of health.






