Fuel availability – impact on homecare delivery
Summary
A snap survey of Homecare Association members was conducted from 30 September to 1 October 2021, to assess the impact of unreliable availability of fuel on their services, a week after problems were first reported.
Responses were received from 108 members, collectively providing care to 55,720 older and disabled people, and employing over 40,000 careworkers, across most regions.
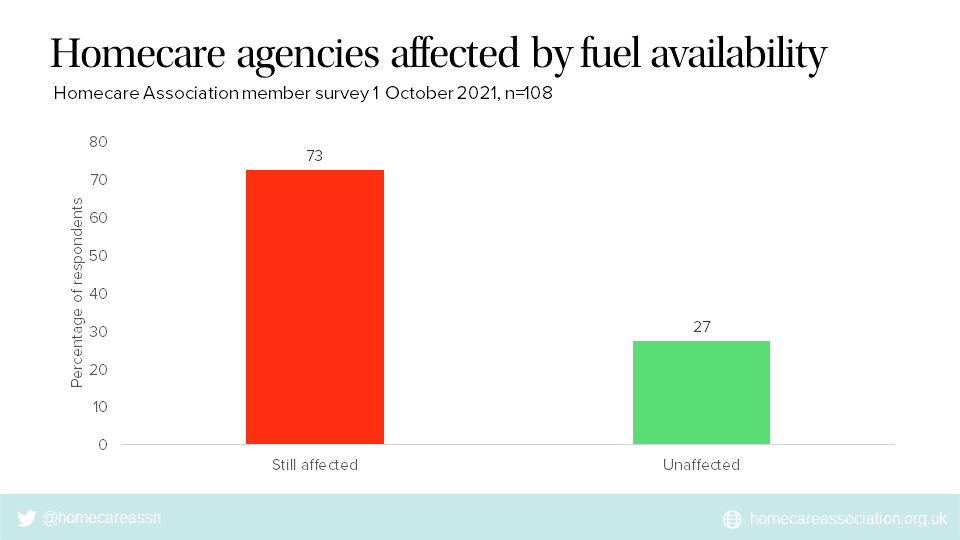
Results revealed that 73% of providers remain adversely affected by problems obtaining fuel, with 27% saying they are now unaffected and it is business as usual.
It was hard to determine any clear geographical patterns, though London and the south-east appear to be more severely affected than northern areas.
Data suggest that fuel availability issues are very localised, with some providers in the same counties reporting that business is unaffected, and others continuing to struggle.
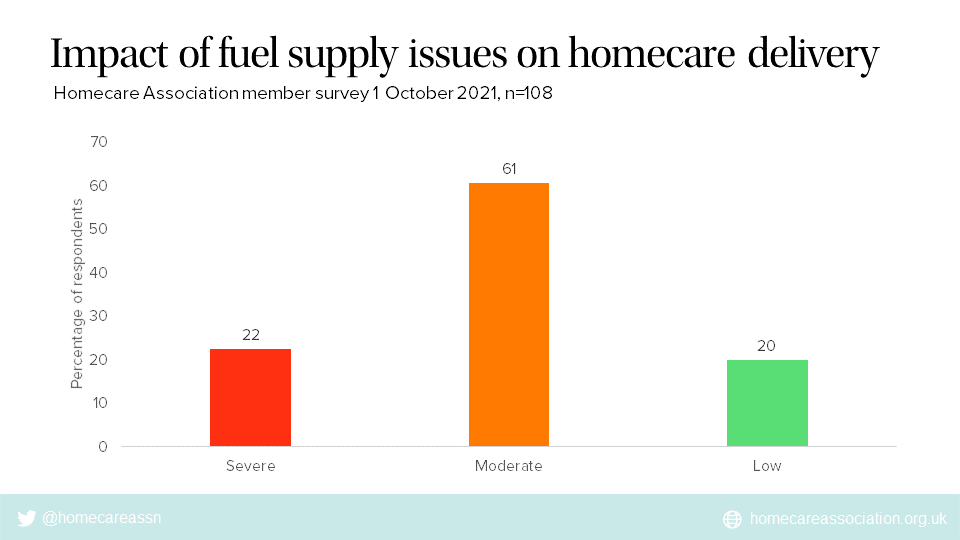
Of the providers still affected by unreliable supplies of fuel, 22% rated the impact as severe; 61% as moderate; and 20% as low.
Providers reported a range of ways, alone or in combination, that homecare services are being affected by unreliable access to fuel.
The most common outcome recorded was that care calls are being delivered late.
Calls are also being reduced or missed, in some cases with adverse effects on the people they are supporting.
Many of the older and disabled people that homecare workers support are alone and entirely dependent on their arrival. Unable to get out of bed, wash, dress, eat or go to the bathroom without help, some face the discomfort of hunger, thirst or incontinence, until their carer appears.
Some are receiving end-of-life care and need time-dependent pain-relieving medication. Others require feeding by a tube, catheter care or wound care, tasks that, increasingly, are delegated to homecare workers, and require substantial training and experience to perform.
ITV reported one example of a 94 year old woman, Vera, being left in a wet bed because her careworker was an hour late reaching her, having had to queue for fuel. This type of issue is heart-breaking and, sadly, is likely replicated up and down the country.
Providers also told us what actions they have taken to mitigate the risks of lack of access to fuel and thus to quality and continuity of care for older and disabled people.
Many providers requested help from petrol stations and from their local resilience forums, most of which declined.
There were a few good news stories and some members have been able to negotiate priority access to fuel at local petrol stations or persuade garage owners to lift the £30 cap.
Most commonly, staff with access to fuel, including managers and office staff, are covering for those without.
Homecare agencies have reviewed risk matrices; reorganised rotas; shared cars; shared information about petrol stations with fuel in online groups; employed staff specifically to queue for fuel; collected fuel in jerry cans; asked careworkers to go out on bicycles; and enlisted family members to cover. They have also revised pay rates; offered wage advances; paid for public transport; and occasionally used remote video calls to check on people.
Homecare providers are deeply disappointed that yet again they have been left to fend for themselves, despite delivering a vital public service to people at home who are unable to manage without support.
In the words of one respondent:
"Homecare is an ongoing, perpetual service. We always go to work. We always deliver care. We run 365 days a year, rain or shine, snow or sun. The services we deliver are literally life or death for service users in many cases. I do not believe there is another service in the country that on any one day is seeing as many visits as home care - not even district nursing let alone fire or police. There's no doubt everyone is doing valuable work but there is no food, no care, no going to loo and no dignity in this situation if we don't work. And still we are left to beg borrow and steal in times of crisis like this. Homecare services need to be included in robust contingency planning. There are too many small providers/franchises etc for any one provider to respond appropriately in these situations".
We call on both central and local government to put the safety and well-being of older and disabled people above all else in situations like this, regardless of what or whom was responsible in the first place.
We need contingency plans that are fit for purpose, which quite clearly we do not have at present.
National coordination of simple solutions, including capping spend at fuel pumps; providing priority time-slots or pumps for essential workers, including homecare workers; and issuing vouchers to prove eligibility could have been quickly achieved, relieving widespread stress and suffering.
How can it be right that in 21st century Britain, we are leaving old people lying in their own urine, or in pain when they are on end-of-life care, when there are simple solutions to help essential workers access the fuel they need? It's a national disgrace.
We offer our heartfelt thanks to each and every homecare worker, manager and leader, for your resourcefulness, resilience, compassion and commitment to the people you support. We know you are running on empty and we are so grateful for all you are doing.
Both older and disabled people and the homecare workforce deserve better and we will not stop until homecare is valued and receives the investment it deserves.
Finding fuel for homecare
Over the last week, many homecare providers across the country have reported difficulties obtaining reliable supplies of fuel for their cars.
A shortage of lorry drivers disrupted supplies of fuel to some petrol stations. As soon as this was reported by the media, the public began panic-buying. Within hours, pumps had run dry.
Homecare workers have struggled through traffic jams, waited hours in queues, and driven miles to obtain fuel. This has created high levels of stress, on top of severe staffing shortages and 18 months of coping with the COVID-19 pandemic.
Desperate to continue providing care at home to at least 550,000 older and disabled people, who are completely reliant on their help, they reached out for support.
Little was forthcoming.
Once again, the government appeared disinterested in the health and well-being of older disabled people.
And once again, they have demonstrated a lack of regard for the 670,000 strong homecare workforce, many of whom are paid by the minute at the national legal minimum wage, as a result of years of central government under-funding of councils.
None of this was a surprise.
What we have learnt this week, though, is that national contingency plans are not fit for purpose.
For political reasons, central government declined to recognise that there was an issue with fuel availability for essential services. Our emails, phone calls and texts to the Department of Health and Social Care went unheeded.
Providers turned to their local resilience forums (LRFs), multi-agency partnerships made up of representatives from local public services, including emergency services, local authorities, the NHS, the Environment Agency and others.
During the COVID-19 pandemic many LRFs supplied PPE and provided invaluable support to care providers.
Most LRFs said they could not help care providers on this occasion. Allegedly, in line with legislation, they cannot invoke civil contingency plans without central government approval.
Providers were thus told to follow their own business continuity plans.
Survey of homecare providers
A week after homecare providers first flagged problems with obtaining fuel, we conducted a snap survey of our members on 30 September to 1 October 2021, aimed at assessing whether issues with fuel availability are still affecting services or not.
Responses were received from 108 members, collectively providing care to 55,720 older and disabled people, and employing nearly 40,000 careworkers.
Of the homecare agencies that responded, 73% reported that they are still adversely affected by difficulties obtaining fuel, and 27% said that they are now unaffected and it is business as usual.
The locations of the providers who responded are shown in the table below, grouped by those unaffected and those continuing to experience difficulties.
It is hard to determine any clear geographical patterns, though London and the south-east appear to be more severely affected than northern areas.
Data suggest that fuel availability issues are very localised, with some providers in the same counties reporting that business is unaffected, whilst others are continuing to struggle.

We asked providers still affected by unreliable supplies of fuel, to rate the impact on their services:
-
22% reported a severe impact
-
61% reported a moderate impact; and
-
20% reported a low impact.
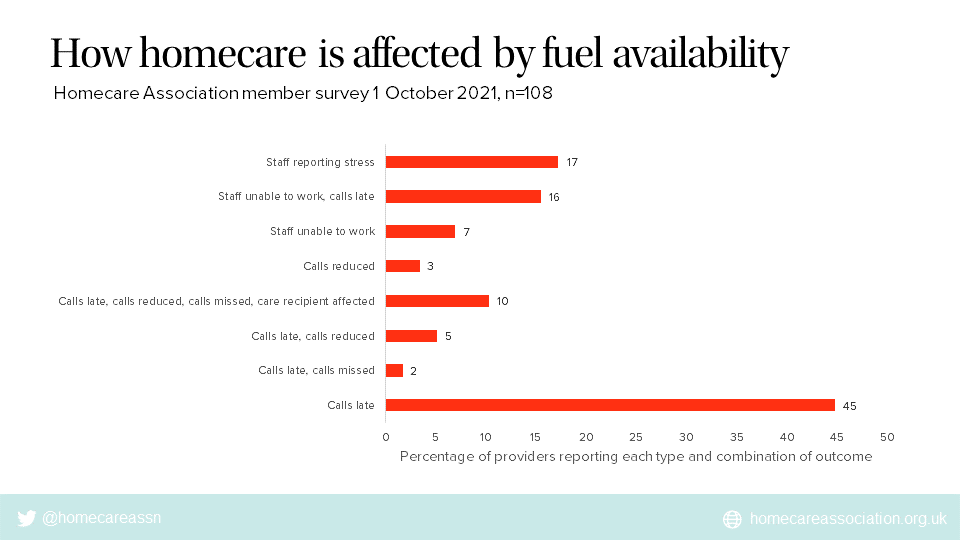
Providers reported a range of ways, alone or in combination, that homecare services are being affected by problems with availability of fuel at petrol stations.
The most common outcome reported was that calls are being delivered late.
Calls are also being reduced or missed, in some cases with adverse effects on the people they are supporting.
Many of the older and disabled people that homecare workers support are alone and entirely dependent on their arrival. Unable to get out of bed, wash, dress, eat or go to the bathroom without help, some face the discomfort of hunger, thirst or incontinence, until their carer appears.
Some are receiving end-of-life care and need time-dependent pain-relieving medication. Others require feeding by a tube, catheter care or wound care, tasks that, increasingly, are delegated to homecare workers, and require substantial training and experience to perform.
ITV reported one example of a 94 year old woman, Vera, being left in a wet bed because her careworker was an hour late reaching her, having had to queue for fuel. This type of issue is heart-breaking and, sadly, is likely replicated up and down the country.
Providers also told us what actions they have taken to mitigate the risks of lack of access to fuel and thus to continuity of care for older and disabled people.
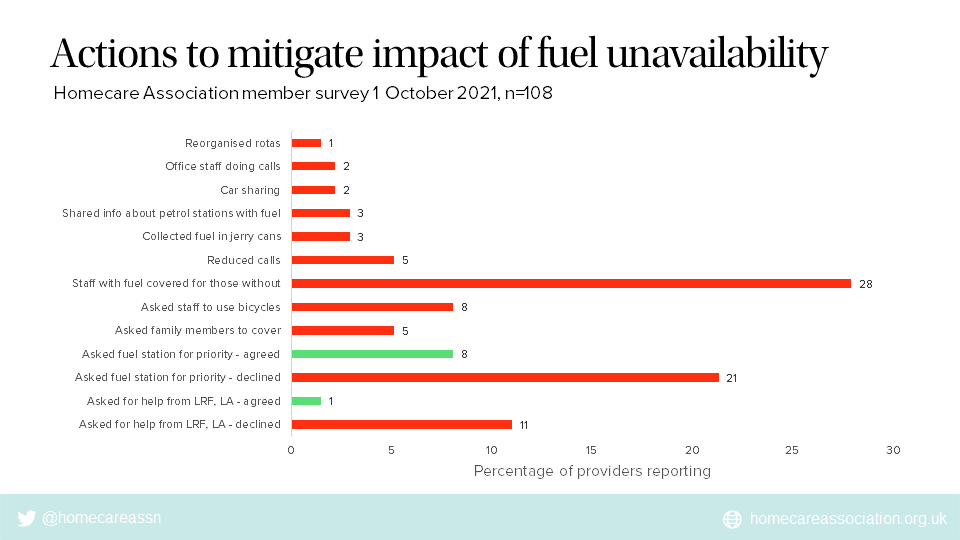
Many providers requested help from petrol stations and from their local resilience forums, most of which declined.
There were a few good news stories and some members have been able to negotiate priority access to fuel at local petrol stations or persuade garage owners to lift the £30 cap.
Most commonly, staff with access to fuel, including managers and office staff, have covered for those without.
Homecare agencies have reviewed risk matrices; reorganised rotas; shared cars; shared information about petrol stations with fuel in online groups; employed staff specifically to queue for fuel; collected fuel in jerry cans; asked careworkers to go out on bicycles; and enlisted family members to cover. They have also revised pay rates; offered wage advances; paid for public transport; provided proof of employment; and occasionally used remote video calls to check on people.
One said their council had turned down a request for planning permission to build an oil refinery in their back garden.
Messages from homecare providers
As the membership body representing and supporting providers of homecare, the Homecare Association acts as a collective voice.
We asked our members what messages they would like us to share on their behalf and key points are below.




Conclusion
As always, homecare providers have proved themselves resourceful and resilient. This has, however, come at a cost, both human and financial. We know they are running on empty.
We call on both central and local government to put the safety and well-being of older and disabled people above all else in situations like this, regardless of what or whom was responsible in the first place.
We need contingency plans that are fit for purpose, which quite clearly we do not have at present.
National coordination of simple solutions, including capping spend at fuel pumps; providing priority time-slots or pumps for essential workers, including homecare workers; and issuing vouchers to prove eligibility could have been quickly achieved, relieving widespread stress and suffering.
How can it be right that in 21st century Britain, we are leaving old people lying in their own urine, or in pain when they are on end-of-life care, when there are simple solutions to help essential workers access the fuel they need? It's a national disgrace.
We offer our heartfelt thanks to each and every homecare worker, manager and leader, for your resourcefulness, resilience, compassion and commitment to the people you support. We know you are running on empty and we are so grateful for all you are doing.
Both older and disabled people and the homecare workforce deserve better and we will not stop until homecare is valued and receives the investment it deserves.