Fuel costs and homecare – impact on service capacity
Findings of Homecare Association member survey, March 2022
Summary
Many people in the UK are deeply concerned about how they will cope with rapidly escalating costs of living, particularly fuel and food price increases. Such inflationary increases are likely to have a disproportionate impact on those with lower income and less secure employment, such as homecare workers.
90% of homecare workers use their own cars or public transport for work. Many are unable to afford newer fuel-efficient vehicles, which means they must pay emissions or clean air charges in cities where they apply. In London, for example, the Ultra Low Emission Zone daily charge is £12.50 for cars. Public transport routes and timetables do not always line up with homecare delivery needs, particularly in the suburbs. In rural areas, public transport is simply not a viable option for homecare delivery. Collectively, homecare workers across the UK are estimated to travel more than 4 million miles per day (homecare visits per day across the UK estimated at 1.5 million, with an average 2.9 miles travelled per visit). Given a high proportion of these visits are by car, fuel costs are significant, particularly in rural areas.
Employers in homecare are acutely aware of the value of their care staff and the pressures they are under and want to ensure they receive fair remuneration, including covering variable costs such as mileage. Operating with increasingly tight margins, though, providers in the state-funded part of the sector have little room for manoeuvre. Providers in the self-funded part of the homecare sector have, in principle, more flexibility to increase charges to clients to increase baseline careworker pay and cover variable costs such as mileage. Average fee rates for state-funded homecare in 2021/22 were £18.57 per hour compared with £24.94 per hour for self-funded homecare. It is unclear, however, whether those paying for their own care will be willing or able to bear increases in charges, as they themselves are also experiencing a rise in the cost of living.
The Homecare Association thus conducted a survey of its members to understand how increased cost of living, particularly a record rise in fuel prices, is affecting the homecare sector. Responses were collected through a self-selecting online survey of Homecare Association member organisations between 11 and 21 March 2022. Responses were received and accepted from 627 homecare providers, large and small, state-funded and private-pay funded, across the United Kingdom. Key points are summarised below, with detailed results reported in the section that follows.
A massive 95% of respondents said their staff had expressed anxiety about current or potential future increases in the cost of living. This concern is widespread, regardless of the location of visits, funding source or geographical region. More than four-fifths (82%) of the sample concluded that the primary concern that staff have expressed on the cost of living was either the cost of fuel or energy bills.
Half of respondents asserted that careworkers had requested an increase in the mileage rate, while more than a fifth (21%) added that careworkers had either given notice, intended to look for work elsewhere or had already done so because they cannot afford to put fuel in their cars.
A North-South divide in England was clearly apparent, with 83% of providers in the North East paying mileage rates of 30p per mile or less, with only 39% in the South West. Regrettably, we have evidence from other work that many homecare workers receive only 10p per mile. Only 2% of providers that responded to this survey were paying above 45p per mile. In contrast, some NHS trusts are now paying community staff 54p per mile, with no reduction at higher mileage levels. There is little justification for treating NHS and care staff differently when they are working on state-funded contracts and serving the same communities. We call for fairness and adequate funding to cover these costs.
| Mileage rate (pence per mile) | Estimated total UK cost (£m) per week based on average miles driven |
|---|---|
| 10 | 3.0 |
| 30 | 8.9 |
| 45 | 13.3 |
| 54 | 16.0 |
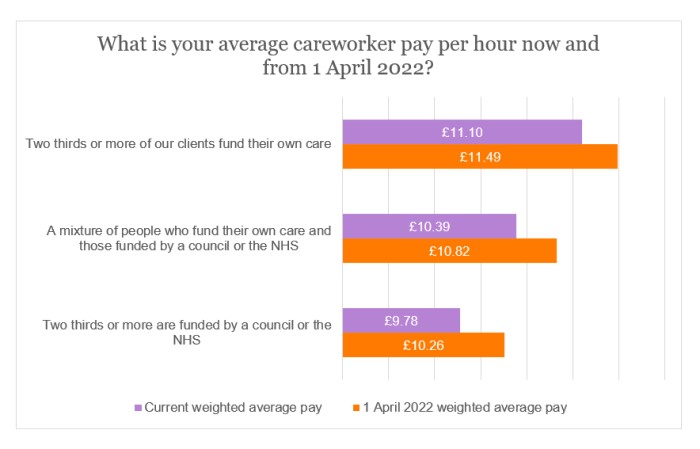
A further divide was noted between careworker pay rates in the state-funded versus self-funded parts of the sector. Using figures as declared by providers, the weighted average hourly pay rate in private-pay providers (£11.10 per hour) is 14% higher than in state-funded providers (£9.78 per hour), though data suggest this gap may reduce slightly after 1 April 2022 (£11.49 vs £10.26 per hour, respectively).
Our findings indicate that an overwhelming 92% of respondents were either concerned or very concerned about the effect of the rise in fuel costs on the financial viability of their company.
The government has allocated insufficient funding to homecare to ensure quality and sustainability of services, preferring to support the NHS instead. Indeed, homecare receives less than 4% of the amount spent on the NHS. This is short-sighted, especially as the NHS is citing collapse of homecare services in some areas as a key cause of delayed discharges from hospital, making elective recovery plans even harder to deliver.
We call on the government to:
- Provide temporary grant funding as a fuel allowance to cover increased costs of fuel for vehicles needed to deliver homecare;
- Provide funding in the short-term to cover emission/clear air charges in cities where they apply and support lease or purchase of electric fleet vehicles for homecare services to enable a reduction in emissions in homecare in the longer-term;
- Provide adequate baseline funding for homecare to ensure that fee rates cover costs and careworkers receive fair remuneration, including full recompense for work-related expenses such as mileage. Such investment is needed to build workforce capacity and reduce unmet need, recognising that NHS hospitals will never succeed in reducing their waiting lists if they cannot free up beds by discharging people back home.
About the collection method and response rate
Responses were collected through a self-selecting online survey of Homecare Association member organisations between 11 and 21 March 2022. Responses were received and accepted from 627 homecare providers, large and small, state-funded and private-pay funded, across the United Kingdom.
In our analysis of answers, we have excluded the very small number of responses stating that they did not know (or preferred not to say) the answer to one or more individual questions.
Organisations completing the survey
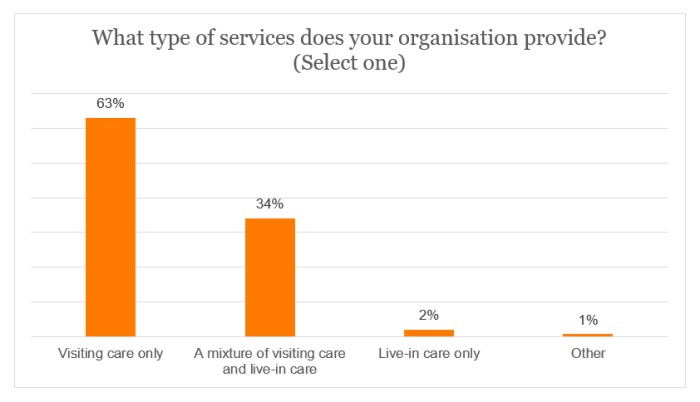
The survey was completed by providers that provided different types of service, as outlined in the graph below. Members that deliver visiting care only or a mixture between visiting care and live-in care had the opportunity to answer all questions in the survey; members that answered ‘Live-in care only’ or ‘Other’ could only questions relating to the cost of living more generally (and not those on fuel/travel).
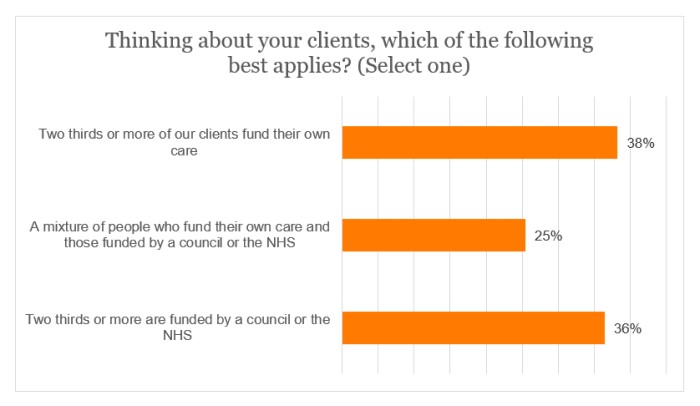
Responses were also received from providers serving either predominantly state-funding or self-funding clients, or a mixture of both.
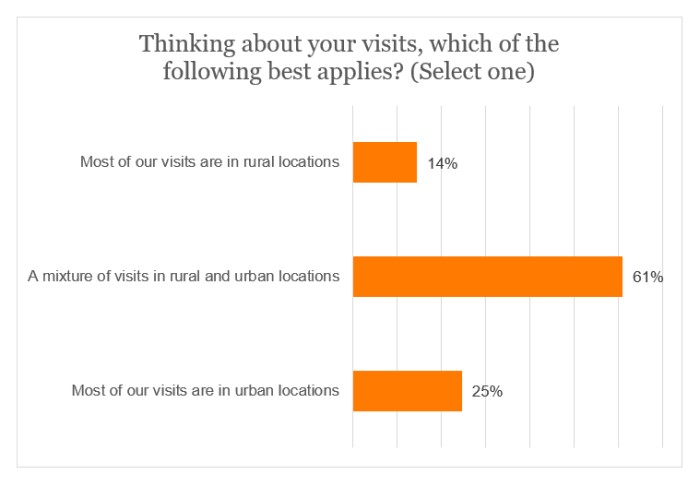
Furthermore, of those delivering either visiting care or visiting care/live-in care, most providers (61%) were conducting visits to a mixture of rural and urban locations.
NB. Data labels on the graphs have been typically rounded to the nearest whole number. Where percentages have been, for example, added or subtracted, exact figures have been used – hence, there may be occasional rounding differences from the graph labels.
Results
Cost of living
A massive 95% of respondents said that their staff had expressed anxiety about current or potential future increases in the cost of living.
As illustrated by the following graphs, this concern is widespread, regardless of the location of visits, funding source or geographical region. However, it is most evident among providers whose visits are predominantly in rural locations, who are state-funded, or are based in the devolved administrations, the North West of England or the East Midlands.
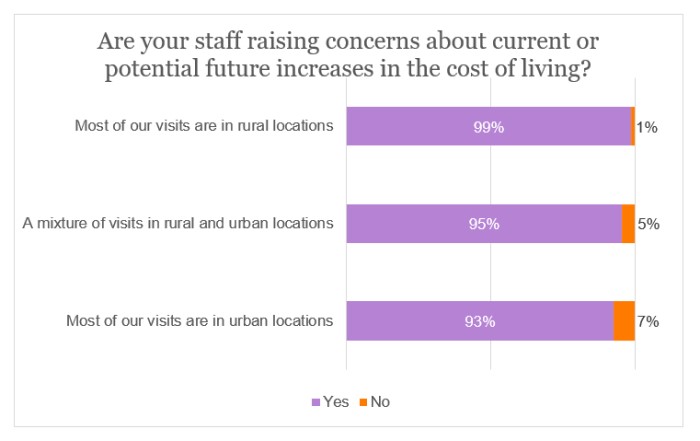
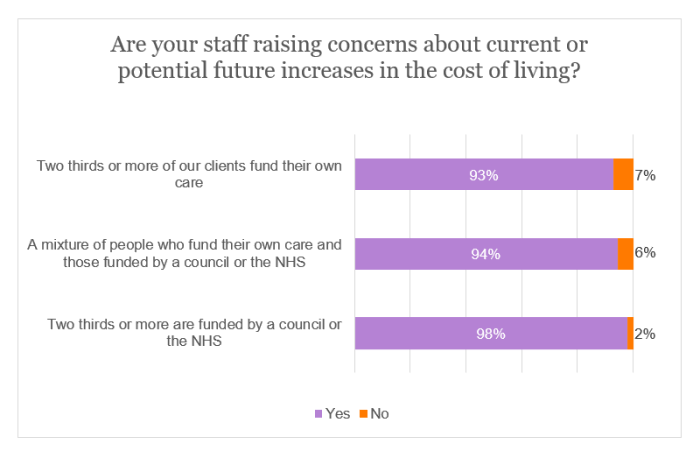
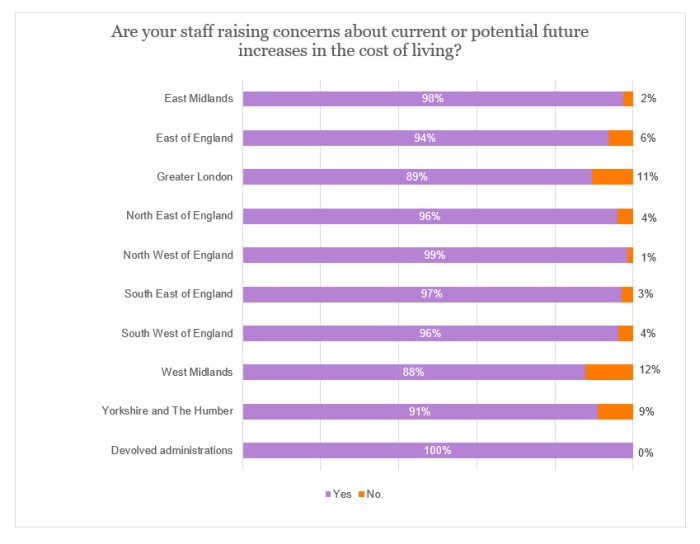
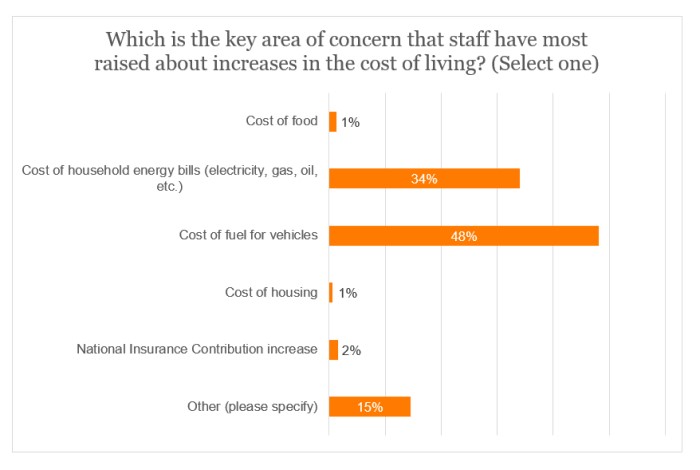
More than four-fifths (82%) of the sample concluded that the primary concern that staff have expressed on the cost of living was either the cost of fuel or energy bills.
15% chose the ‘Other’ category, with the responses typically being either a mixture of the options presented in the graph below, or all such options. The cost of childcare was also referred to. The following comments were made:
Fuel and food are what carers are noticing now. A lot of carers live month to month, they will not feel the effect of the upcoming increases to council tax, [the] new energy cap starting and NI increase until it hits them. It is going to be a very tough few months for carers and, after the last 2 years, I am not sure how they will react/cope. We have limited scope to increase rates as local rates have been capped for our work.
Some staff have threatened to leave if we do not give them work [to] which they can walk or pay them at least 45p per mile to cover their mileage costs.
We have experienced a huge increase in careworkers asking for advances on their monthly pay because they simply cannot make ends meet.
Careworker response
Half of the sample asserted that careworkers had requested an increase in the mileage rate, while more than a fifth (21%) added that careworkers had either given notice, intended to look for work elsewhere or had already done so.
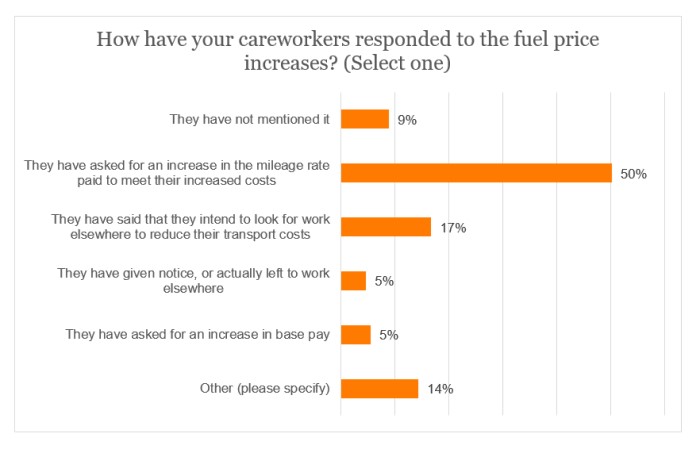
14% of providers chose the ‘Other’ option and were invited to provide comments. The general feeling was one of genuine anxiety and concern about this issue, as careworkers sought assistance. Some had already increased their mileage rate, while others had received a mixture of responses from careworkers. The comments included the following:
We have had a mixture asking for an increase, looking to leave, and have already had resignations. The resignations equate to 10% of our workforce - when recruitment is difficult, this will affect staffing levels.
10% of staff have directly asked for either a pay rise or a rise in the pence per mile expense! 5% of those staff state they are actively seeking jobs where they don't have to drive (or the drive is limited to a single location). YIKES!! This survey is so well-timed. We (the sector) need help.
We have had numerous calls about increasing cost of fuel and we will have to increase our mileage payments with the next NMW increase. We have not had confirmation of the local authority increase as yet but, since 2019, the margin for this work has been eroded by 6% as previous NMW increases have not been met. An additional 5p per mile on fuel impacts our payroll by circa £6500 pcm (delivering around 1600 hrs of care per week) which will very soon make this work unsustainable.
In spite of increasing our fuel pay to account for car mileage and public transport costs and paying other benefits, staff are still leaving as it is not enough and there are other jobs out there that require less commitment and no/less travel.
They have asked for an increase, we increased their hourly rate in February (2 months earlier than planned) owing to the sudden rise in utilities. This fuel cost coupled with the forthcoming increase in NI has left a lot of staff feeling bad and questioning the worth of them going to work.
When breaking the data down by visit location, almost three-fifths (59%) of respondents who predominantly visit rural locations claimed that staff had sought a rise in the mileage rate – a statistic that is 21 percentage points higher than that for those mainly visiting urban locations. Indeed, 18% of the urban-location sample stated that the issue had not even been raised by careworkers.
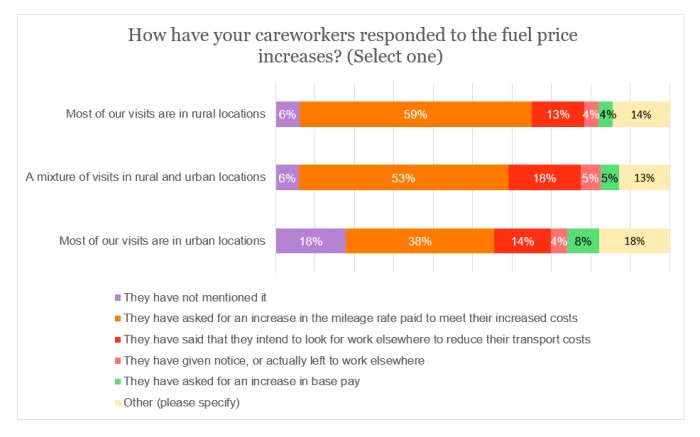
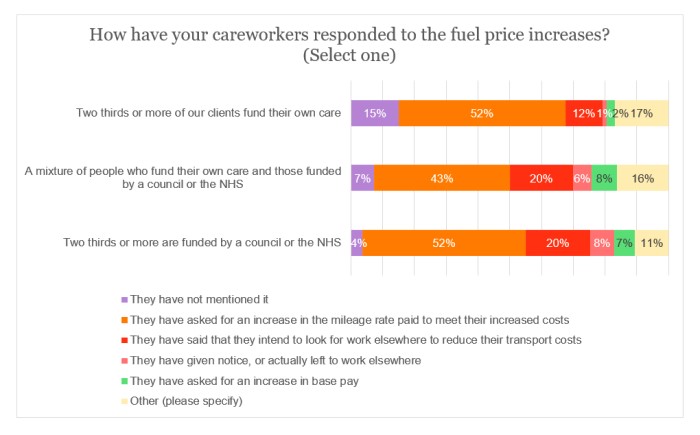
When rounding to the nearest whole number, an equivalent proportion (52%) of providers in the state and self-funding sectors said that careworkers had requested a mileage rate rise. However, more than a quarter (28%) who are funded by a local authority/NHS elucidated that careworkers had either left to work elsewhere, were looking to do so, or had provided notice; the associated percentage for those reliant on self-funders was just 13%.
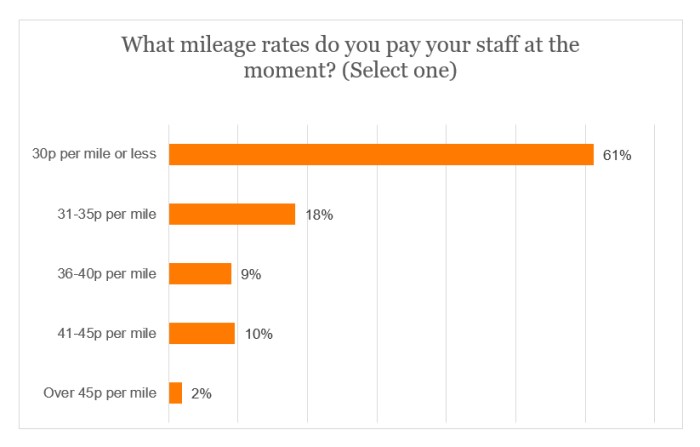
Mileage rates
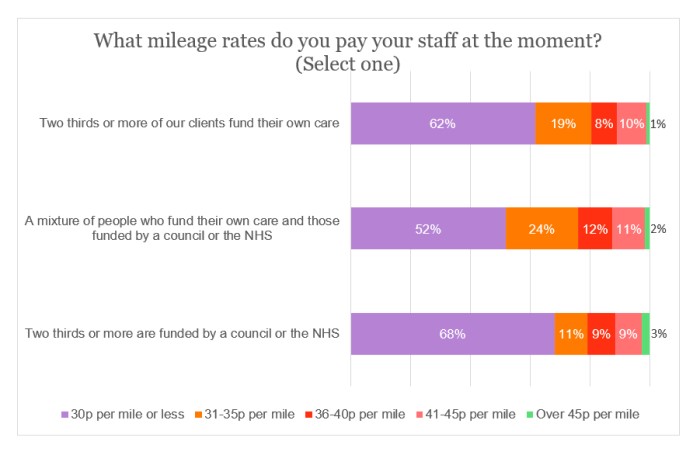
Just over three-fifths (61%) of respondents were paying mileage reimbursement to their staff at a rate of 30p per mile or less. In contrast, only 2% were paying above 45p per mile.
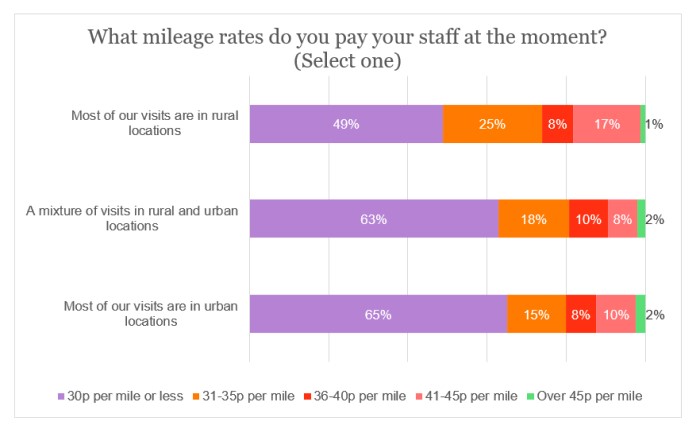
It was noticeable that the mileage rate offered by providers predominantly visiting rural locations was better than those mainly attending urban locations. Less than half (49%) were paying mileage expenses of 30p per mile or less in rural locations; the respective figure in urban locations was close to two-thirds (65%). Similarly, the proportion paying more than 40p per mile was six percentage points higher for rural-location providers.
There was a difference of seven percentage points between providers paying 30p per mile or less who are predominantly state-funded compared with those who are mainly reliant on self-funders. Despite this, a fractionally higher proportion in the state sector were paying more than 40p per mile.
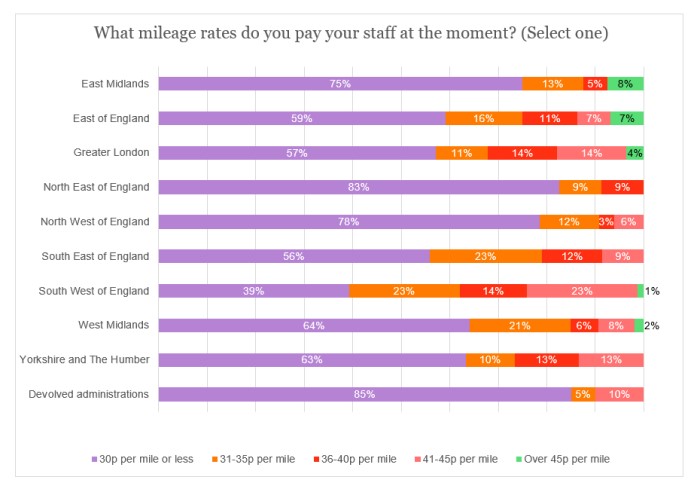
Evidence of a clear North-South divide in England was apparent for providers paying 30p per mile or less, with percentages ranging from 39% in the South West up to 83% in the North East. Moreover, almost a quarter (24%) of South West respondents were paying above 40p per mile, while not a single provider in the North East who completed the survey was able to offer this rate. Within the devolved administrations, 90% of providers were offering a mileage rate of 35p per mile or lower.
Average pay rates
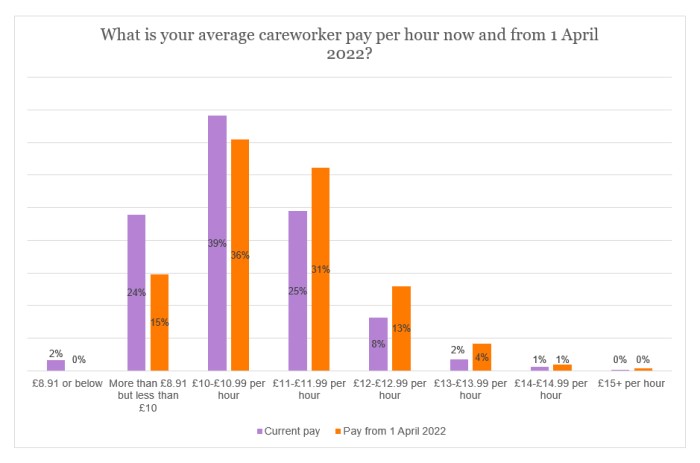
Respondents were asked to provide their average pay for careworkers, now and from 1 April 2022. To ensure a fair comparison, only members who supplied both rates are included in the following analysis (some were still awaiting to hear confirmation on fee rates from their local authority). In addition, providers delivering live-in care only are excluded (rates are given as daily or weekly figures, and there is an insufficient number to analyse). The data was also cleaned before analysis – for example, if respondents provided a range of rates, the lowest rate was used.
At present, almost two-thirds (65%) of providers are paying their careworkers an average rate of £10.99 per hour or below, with 39% asserting that their rate is between £10 and £10.99. From 1 April 2022, there is a change, however, with an increase of 11 percentage points for respondents paying an average hourly rate of between £11 and £12.99.
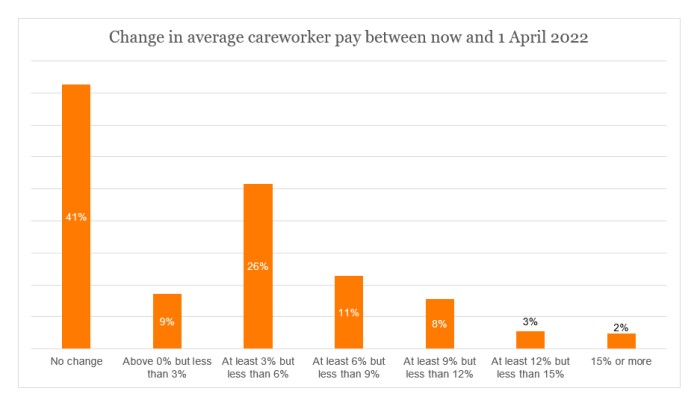
Just over two-fifths (41%) reported that there would be no change in their average pay to careworkers between now and 1 April 2022 (although it must be stressed that this does include a small proportion who stated that they had already increased their rates). Around a quarter (26%) asserted that their pay would rise by at least 3% but less than 6%.
We can also compute hourly weighted averages when breaking the data down by location of visits and funding source that consider the number of careworkers as stated by survey respondents (i.e. more weight is given to the average rates of providers who have a higher quantity of careworkers).
The following chart shows that the current weighted average pay for careworkers where visits are predominantly in rural locations is £10.44 per hour, around 2% higher than for urban locations. However, the gap will narrow slightly from 1 April 2022, with only 12 pence between the two weighted averages.
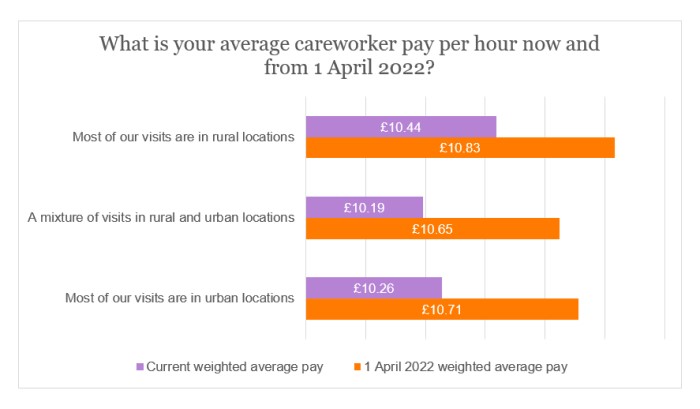
The difference in weighted average pay rates between the self-funding and state sector, however, is much more profound. Indeed, as it stands, the weighted average hourly rate in the self-funding sector exceeds the state sector by 14%, although there will be a marginal improvement from 1 April 2022 (down to 12%).
Financial viability
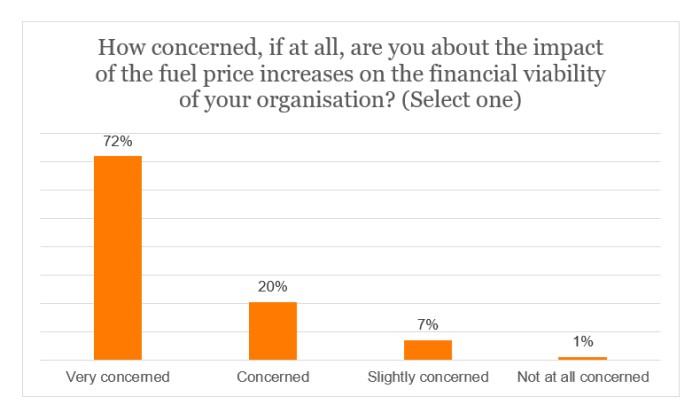
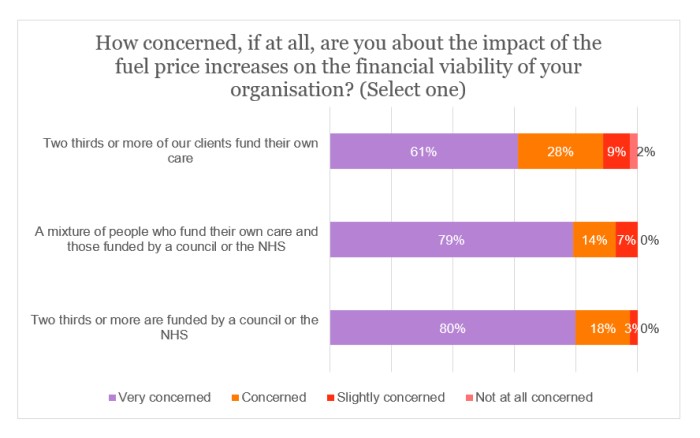
An overwhelming 92% of respondents were either concerned or very concerned about the effect of the rise in fuel costs to the financial viability of their company. Indeed, 72% alone were very concerned.
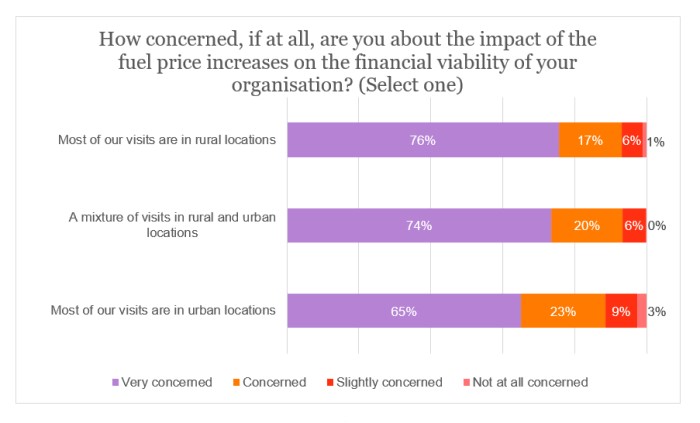
More than three-quarters (76%) of providers whose visits are mainly in rural locations were very concerned – a proportion which exceeds that for urban-location respondents by 10 percentage points.
Most respondents (61%) in the self-funding sector were very concerned about the present situation. However, the respective proportion in the state-funded sector was 80% (with 97% either concerned or very concerned).
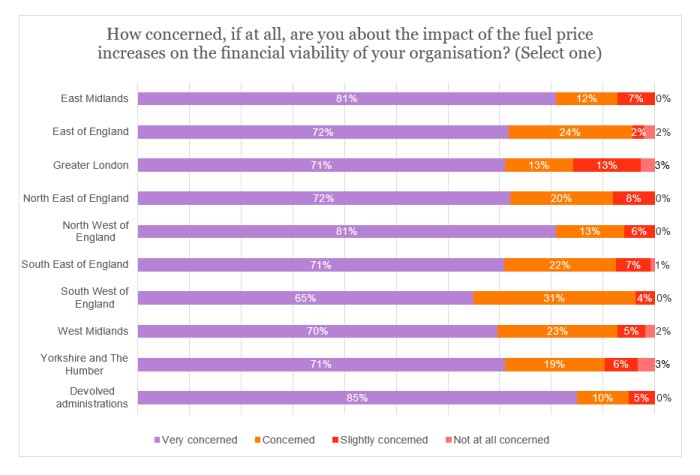
Anxiety about the rise in fuel prices was clear across the United Kingdom, with most respondents in every region expressing that they were very concerned. 85% of the sample in the pooled devolved administrations offered this view, likewise 81% in both the East Midlands and the North West of England. It was also noticeable that, in seven of the UK’s 12 regions (with the devolved administrations split), not a single respondent was ‘not at all concerned’ about the issue.
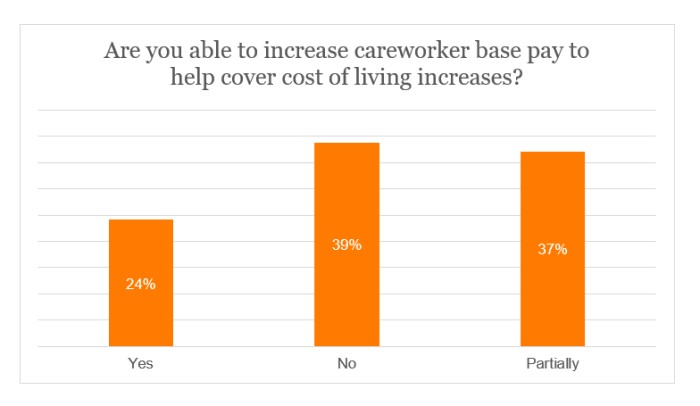
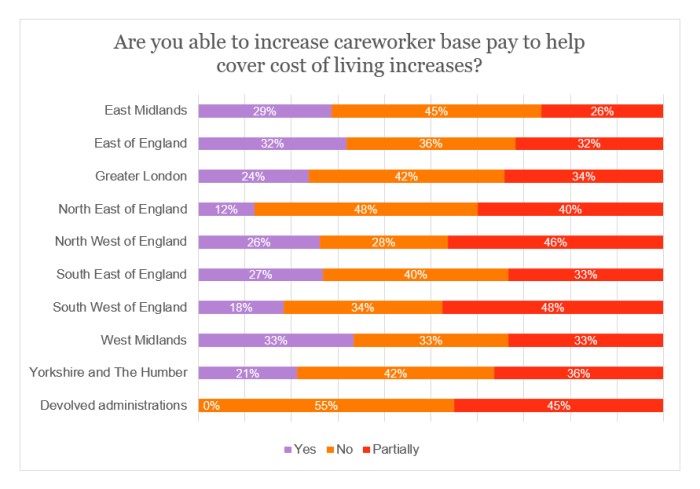
Increasing careworker pay
Just under a quarter (24%) of respondents asserted that they would be able to raise the base pay for careworkers in light of the increase to the cost of living.
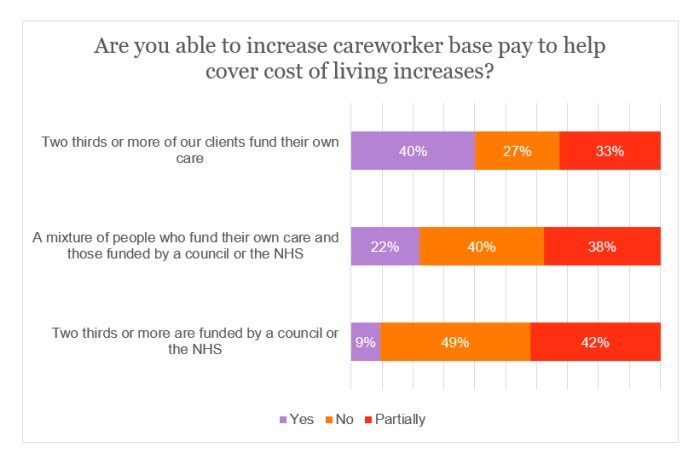
There was a stark contrast when breaking the data down by funding source. Indeed, 40% of providers who are mostly reliant on self-funders would be able to raise pay, compared with only 9% for those predominantly funded by the state.
There was no region in which more than a third of respondents stated that they could increase careworker pay. According to the sample, the issue was most acute in the devolved administrations, North East of England and South West of England.
Ultra Low Emission Zone (ULEZ)
We asked our members (where applicable) about the planned expansion to make the ULEZ London-wide, and how they or their local commissioners are managing this additional expense.
For those affected, responses included:
- Adapting to use public transport.
- Registering vehicles for automatic payment and pay for staff to use this service as additional expenses
- Increasing the cost to service users.
- Lack of support/concessions from local authorities.
Two of the comments made were:
This is going to [be] disastrous because many of our staff will need to purchase new vehicles which is unlikely to be affordable for most.
We are struggling as carers are refusing to go into these areas with their cars. Ealing Borough have not mentioned this or any other increases for this year. It is as if they don't live in this country at the moment and have not realised the increase in costs of everything around them.
Other providers referred to, for example, the new Zero Emission Zone (ZEZ) in Oxford, similar schemes in Bath & North East Somerset and Bristol, and Birmingham’s Clean Air Zone (CAZ).
A provider in the South East of England, affected by Oxford’s ZEZ, asserted that they will ‘not pick up work in these areas’. Meanwhile, a West Midlands member stated that they ask the service user to pay for parking in the CAZ in Birmingham and only send ‘staff who use public transport’ to visit such users.
Government interventions
Respondents were presented with a range of potential government interventions to tackle the current fuel prices increase and then asked to rate each on a scale between 1 (‘not at all helpful’) and 10 (‘extremely helpful’). The results are depicted on the chart below, with data labels only shown for those answers rated either ‘1’ or ‘10’.
Apart from subsidised access to electric vehicles, the sample thought that it would be extremely helpful to enact each intervention (i.e. most respondents chose this option). However, the extent to which this was the case varied significantly – just over a third (34%) thought that prioritised access to fuel pumps would be extremely helpful, compared with more than four-fifths (82%) for additional grant funding until prices go down (by far, the most popular proposal).
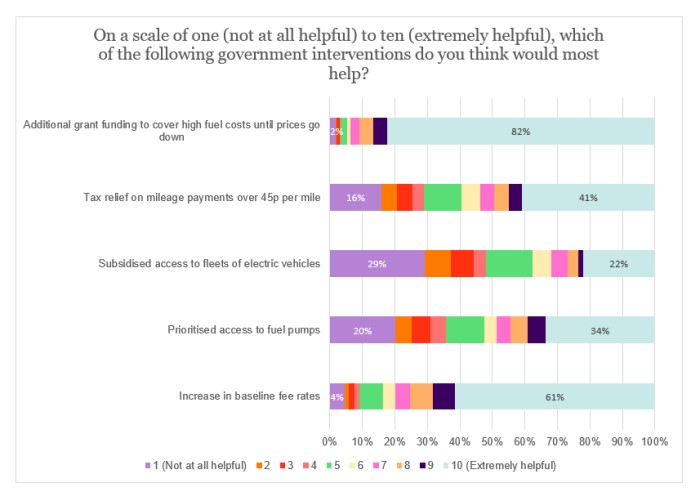
Respondents were also able to postulate other government policies that would help the sector. These included:
- Reduce fuel duty or VAT on fuel.
- Discounted fuel rates for careworkers.
- Tax relief on mileage payments.
Contingency arrangements
Only 4% were aware of their local authority having contingency arrangements so that careworkers can get fuel in the event of queues or shortages. As illustrated in the following graph, this was evident across all regions.
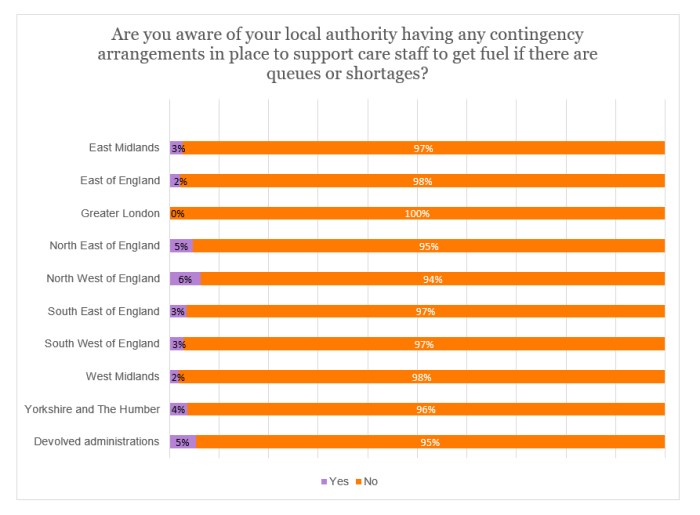
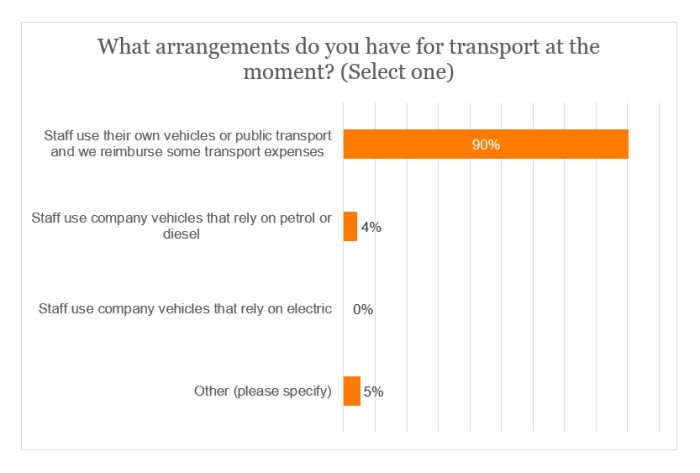
Transport arrangements
Currently, the staff of 90% of respondents use their own vehicles or public transport, with expenses being paid.
Within the ‘Other’ category, some providers mentioned that their present arrangements were a mixture between staff using either their own vehicles or company vehicles. One respondent asserted that they had ‘no possible use of public transport or walking/cycling as distances are too great.’
No sample member claimed that their careworkers use electric, company vehicles – another respondent noted that they cannot ‘justify electric vehicles owing to the rural locations’ that they cover.
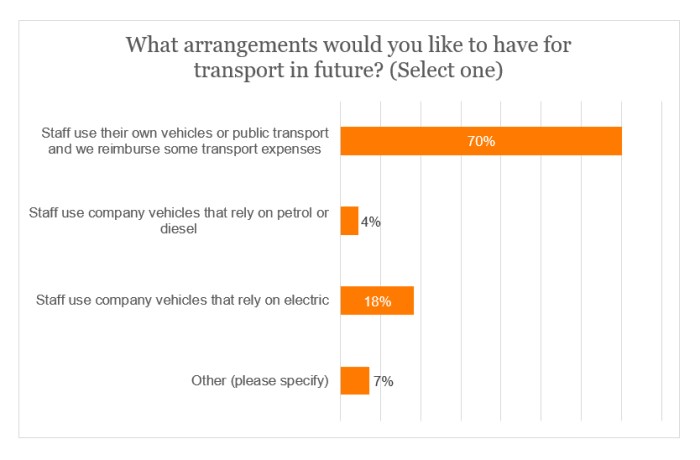
Regarding future arrangements, almost a fifth (18%) opted for electric, company vehicles, with a drop of 20 percentage points in staff using their own vehicles or public transport.
In the ‘Other’ category, respondents alluded to a mixture of the options presented, the use of bikes or staff using their own electric vehicles. Among the comments made were:
The government should give a 25% refund to anyone who buys an electric car and also grant them tax relief on the interest payments on any loan taken out to buy an electric vehicle, just as they used to grant tax relief on the interest on mortgage repayments (MIRAS).
Funding for support of company vehicles so carers have vehicles to suit their role, i.e. electric in urban areas where charging points are readily available and affordable. In mixed and rural areas, [there should be] access to efficient petrol vehicles.
We are introducing a salary sacrifice scheme to our workforce so they can get into a brand new electric vehicle, which is deducted each month from their gross pay, therefore saving them on tax and national insurance. Although we do not yet know how many staff members will sign up to this.
Of those respondents who did foresee barriers to moving to their preferred transport arrangements, the overwhelming majority mentioned the cost involved (for example, of electric vehicles, insurance, and electricity/fuel), with some of the sample alluding to the fee rates being paid by local authorities. The lack of charging points for electric vehicles was also an issue. Here is a selection of the most salient comments:
Base rate funding does not allow the replacement of petrol vehicles to electric which are at minimum 2 to 3 [times] the cost per month to lease.
Whilst we would welcome support for fleet vehicles in many of our services, this would not solve the issue. Fair pay and fair mileage rates need to be funded through improved commissioning and fee rates to reflect actual costs of care.
We have had to introduce a travel charge to clients in addition to the hourly care rate.
I have written to DHSC on several occasions asking about [the] possibility of home carers having a mobility scheme akin to that for disabled drivers, and which would be based on a minimum number of miles travelled for the job, and an employee contribution for personal mileage. There are several models that could be adopted. Attracting carers to [the] homecare profession would be greatly helped by a company/national car scheme.
Subsidised car tax, MOTs, car insurance [and] even driving lessons to help get more carers into the industry.






