On 22 July 2025, the Home Office changed the Immigration Rules, stopping care employers from recruiting careworkers from overseas.
We’re concerned this change could worsen workforce shortages in the care sector. We’re also concerned this won’t address the exploitation some international careworkers already in the country experience.
The Labour Government argues that care providers should recruit locally because:
- Care work is low-skilled work.
- Employers should fund local training and recruit locally.
- The sector’s vacancy rate is stable.
- Existing internationally recruited careworkers can stay (and it is assumed that they will stay).
- Care providers and criminal agencies have brought too many careworkers into the country and employers can now recruit from a ‘pool’ of workers whose original jobs didn’t exist or whose original sponsors have had their licences revoked.
- There are regional hubs in England that will support careworkers who need to find a new sponsor.
- The Fair Pay Agreement will make it easier for care employers to recruit locally in the medium to long term, so they will not need to recruit internationally.
Here are twelve key reasons we think that the Government's line of argument is not correct:
1. Care work is not low-skill work
Care work requires a huge amount of kindness, empathy, responsibility and ability to think on your feet when working alone. Care jobs can also involve undertaking technical tasks. There are many, but some of them include: helping people with medication, catheter care, skin integrity, communicating with people in sign language or Makaton, understanding the needs of people with dementia or supporting people in the last days of their life.
If you needed someone to support or care for you, your friend or family member, you wouldn’t want to settle for just anyone (though everyone is finding recruitment hard, including direct payment users). Skilled international staff are a vital part of our workforce, helping the UK support people with care needs.
2. This is not just about care homes
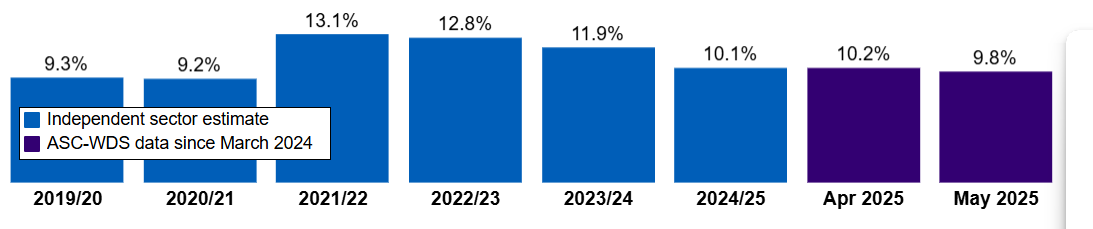
Media headlines focus on the impact of immigration changes on care homes, which is important. However, half of the total jobs in the care sector (580,000 of 1,705,000 filled posts) are homecare roles where careworkers support people in their own homes. Vacancy rates in homecare at 9.8% are higher than in care homes where vacancies stand at 3.6%.
Figure 1: Skills for Care vacancy rate trend for homecare (source)
3. Serious concern and low morale among existing overseas care staff
After hearing about the Immigration White Paper, many careworkers felt uncertain about how the changes would affect them, or if they could apply for settlement. We know this had a negative impact on the morale of existing overseas staff. The Department of Health and Social Care has since clarified that careworkers already in the UK can continue to work as careworkers and renew their visas until they are able to apply for settled status.
Despite this, we know overseas careworkers, who are still struggling with uncertainty about what their situation is, feel worried about their circumstances and about what policy changes are coming.
4. The Fair Pay Agreement will not happen in the next few months
The Government has committed to introducing a Fair Pay Agreement for adult social careworkers. Ministers say this will improve retention and recruitment of domestic workers into the sector.
To enable this to happen, the Government road map for the Employment Rights Bill says they plan to bring forward regulations to establish an Adult Social Care Negotiating Body in October 2026. Once established, negotiations between employee and employer representatives must still follow to reach an agreement.
Although margins in homecare are perilously tight and the public sector buys 80% of homecare, H.M. Treasury has not announced funding to support this agreement yet.
5. The Fair Pay Agreement may not solve our recruitment issues
In the last five years, Scotland, Wales and Northern Ireland have all brought in policies so careworkers get paid more than the statutory minimum wage. This has not solved the workforce shortages in the care sector in those administrations. There are similar examples in other countries, including Sweeden highlighting other factors of working conditions also need consideration. Wage increases are important and welcome (if funded), but they’re not enough. The Government must develop a proper workforce strategy for the social care sector.
6. Can the 39,000 displaced careworkers fill the vacancies in the sector?
Skills for Care reported 131,000 vacancies in the care sector in 2023/24. The total number of displaced workers make up around 30% of this figure.
The Work Rights Centre have found the regional hubs set up to support displaced workers have only matched 3.4% of displaced staff to new roles. Even if all 39,000 displaced careworkers found roles in the sector, we’d still have 92,000 vacancies.
Providers report significant issues when using the hubs. It is not easy for employers to find staff who are able to drive, have the right skills and are in the right area to take up homecare roles available.
7. Many international workers facing difficulties are not ‘displaced’. The Regional Hubs may not help these workers

We continue to hear concerns from providers who hear from sponsored staff whose primary sponsor is not giving them enough hours of work to meet their visa conditions. In some cases, this is deliberate. In other cases, employers lose work unexpectedly. Losing work unexpectedly is not unusual in homecare, and is often driven by public sector commissioners not guaranteeing work to care providers.
Some employees in this situation are afraid to report their sponsor because their ability to work legally in the UK depends on their sponsor. They are also afraid to ask for help from recruitment hubs or other Government agencies. This is usually because they are concerned speaking up will affect their visa, affect their colleagues, lead to them having no income or lead to immigration enforcement. This is particularly difficult when they also have no recourse to public funds.
Where they do make contact, regional hubs are prioritising workers that are displaced by sponsorship licence revocation. This means that in some parts of the country workers that are not getting enough hours from their current employer can access help from hubs to find alternative jobs, and in other areas they cannot (depending on the number of workers in that area affected by sponsorship licence revocations).
Without a safe way to raise concerns about employers, these workers are likely to remain exploited and silent.
8. "Care worker visas only started in 2022"
While it is true that careworkers have only had access to Skilled Worker visas since 2022, in 2021, senior careworkers had access to the Skilled Worker visa route to recruit from abroad. Now they do not.
The workforce situation was significantly different when the UK was part of the EU. The loss of freedom of movement has changed the employment landscape and social care's ability to recruit. When freedom of movement ended during the pandemic, the sector saw more competition for domestic recruits from other sectors such as retail, hospitality and healthcare. This (amongst other factors, related to the pandemic) made domestic recruitment harder. It was because of this difficulty that careworker visas were introduced in 2022.
To imply that the care sector managed fine before the pandemic, so can now, is to ignore the significant changes that have happened in the last five years (including the pandemic and Brexit).
9. Changes in UKVI processes caused the fall in care visas issued from 2023 to now, not enforcement. Difficulties assessing Certificate of Sponsorship (CoS) applications are driven by public sector commissioning practices
Figure 2: Monthly applications for ‘Skilled Worker’ and ‘Health and Care Worker’ visas, January 2022 to June 2025 (source)
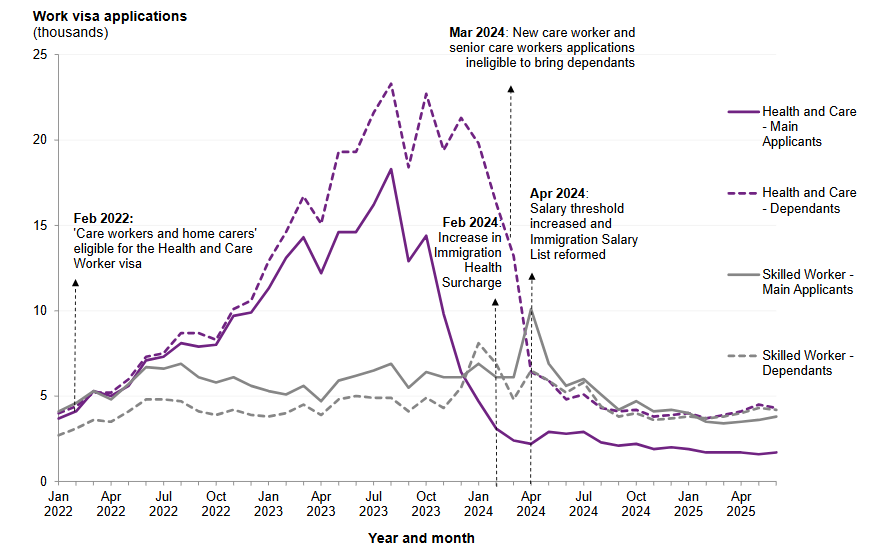
In late 2023, before the current Government announced further changes to the visa system, the Home Office started to apply a more rigorous ‘genuine vacancy test’ to applications for Certificates of Sponsorship. This required care employers to demonstrate they had the hours of work available to employ a sponsored worker. In many cases, even large, legitimate employers with a high volume of work still struggled to prove they had guaranteed hours available. This is because their contracts with the NHS and local Government do not guarantee them any hours of work. This is despite the fact they could prove they had consistent work available.
The rigorous approach from the Home Office reduced the number of overseas workers. We believe this approach has not worked and does not constitute effective enforcement. A care provider has challenged the use of the ‘genuine vacancy test’ in this way successfully in court.
It is vital the Government address exploitation, but there is a need for joined up thinking between public sector commissioning approaches and UKVI requirements.
10. Care staff availability is a regional issue
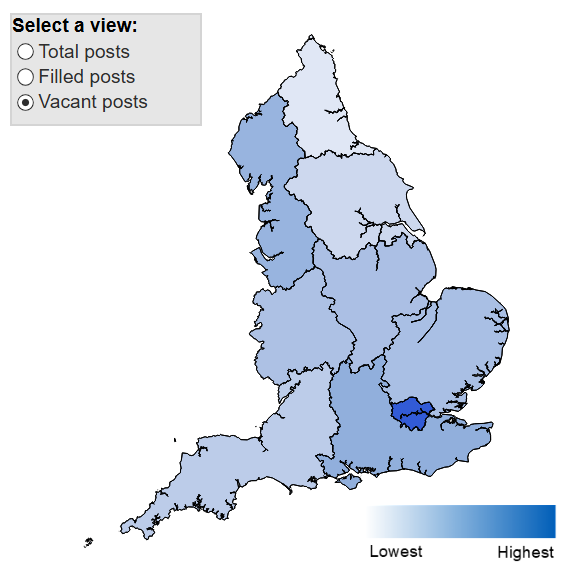
There is a huge variation across the country in the proportion of the homecare workforce on sponsored visas. According to Capacity Tracker, a tool the Government uses to collect data from care providers, this ranges from around half the workforce in some areas to very low levels in others. Consequently, the loss of the option to recruit staff from overseas will affect some areas, like London, more substantially than other regions. Some of our members have high numbers of overseas workers, who they are dependent on to deliver quality services.
To complicate the regional reliance on international recruitment, sources of recruits now that route has closed also vary regionally - displaced workers are concentrated in certain regions, and not necessarily in those areas with the most vacancies. Measures to attract domestic recruits will also vary in their affect regionally – for example, a national Fair Pay Agreement (when reached) could have less effect in London, where the cost of living is high.
It is vital that the Government develop a strategic workforce plan that is sensitive to regional differences.
Figure 3: Skills for Care visualisation of homecare vacancy density across English regions (source)
11. The Government incentivises poor employment practices in the care sector via commissioning practices
Hammersmith and Fulham Council wrote to us to say that in 2025/26 they propose to pay £18.76 per hour for homecare. This means the fee rate they pay homecare providers is less than a care worker wage and the following statutory employment costs:
- The statutory minimum pay (National Living Wage) is £12.21 per hour.
- Wages for travel time (8 minutes on average) would cost £2.75.
- Employers' National Insurance and legally required pension contribution cost £2.54.
- Holiday pay would cost £1.95 (at required 12.07%).
Combined, this is £19.45 – and this doesn't cover sick pay, training time, travel reimbursement (like mileage), or notice and suspension pay.
This also doesn't cover any running costs of the homecare business. These costs are required to cover compliance with care regulations. For example, wages for the Registered Manager, care supervisors, care coordinators and other office staff; non-staff training costs; recruitment; CQC fees; insurance; digital care record systems, other IT and telephony; costs of rent, rates, utilities for a registered location; PPE; legal, financial and other professional services; and a small surplus for resilience and investment.
Providers cannot cut back on these costs and comply with all legislation because they are almost all statutory requirements.
80% of work is paid for by the public sector and where that approach drives a race to the bottom on low fee rates it rewards employers that can deliver for less – often by cutting costs in ways that don’t comply with employment regulation. One example could be not paying careworkers for travel or training time.
These practices can make domestic recruits reluctant to work in the sector and simultaneously can leave international recruits vulnerable to exploitation as their visa is tied to their employer and they have no recourse to public funds. This can make them reluctant to raise issues as they fear deportation or destitution. Closing the visa route does nothing to address either of these issues. Meanwhile, responsible employers struggle to secure work from local authorities at sustainable rates. We are hearing more reports of commissioners moving work to cheaper providers, eroding employment conditions.
12. Most of the care sector cannot afford to pay staff better and pay for extra training without additional funding
We calculate £32.14 is needed in 2025/26 to cover a minimum operational standard whilst paying careworkers National Living Wage for all of their working time.
The Government purchase 79% of care, often at prices lower than this.
Our research shows that:
- 27% of local authority contracts in England fall below the minimum direct employment costs of employing a careworker at £12.21/hour, including travel and training (i.e. the direct wage costs without including management, office and other costs).
- Six councils in England, including Labour-led authorities, offered 0% uplift in 2025–26, despite 10–12% cost pressures on providers.
- The average council fee rate is just £24.10/hour, compared to the Homecare Association's Minimum Price of £32.14/hour.
- Only 1% of contracts meet or exceed the legal and operational threshold for sustainable, safe care (i.e. meet the minimum price, including wage costs, management, office and other operational and regulatory costs).
In this kind of operating environment, many employers do not have the spare resources to develop new recruitment and training initiatives or to reward people who work to progress their careers. This means that existing groups of domestic jobseekers who may be interested in a role in care cannot be reached. Those wanting to develop their career in care may leave the sector to advance their prospects in the NHS or elsewhere. It is not enough to tell employers to offer more training without funding being available for this.
Our recommendations for change
We are calling for:
- A credible workforce plan – developed with the sector, to ensure there will be enough careworkers available to support the UKs ageing population
- Processes that enable protection and redeployment of sponsored workers without enough hours as well as those who are displaced.
- A National Contract for Adult Social Care - Legally binding minimum fee rates that prevent the underfunding that drives exploitation
- Shift-based commissioning – Paying workers for shifts, moving away from minute-by-minute purchasing to provide workers with guaranteed hours and more security of income
- Geographic commissioning zones - Ending the fragmentation that results in inadequate hours for each provider, threatening worker income and provider sustainability.
- Multi-year funding settlements - Enabling sustainable workforce planning and development
- Coordinated regulatory response - Ensuring all agencies work together to identify and prevent exploitation
